Physiotherapy and Sports Injury Clinic in Swansea & Reading
Expert care for musculoskeletal, sports, and men’s health conditions, all under one roof. Clinic locations in Swansea and Reading.
About us
Redefining Musculoskeletal Care
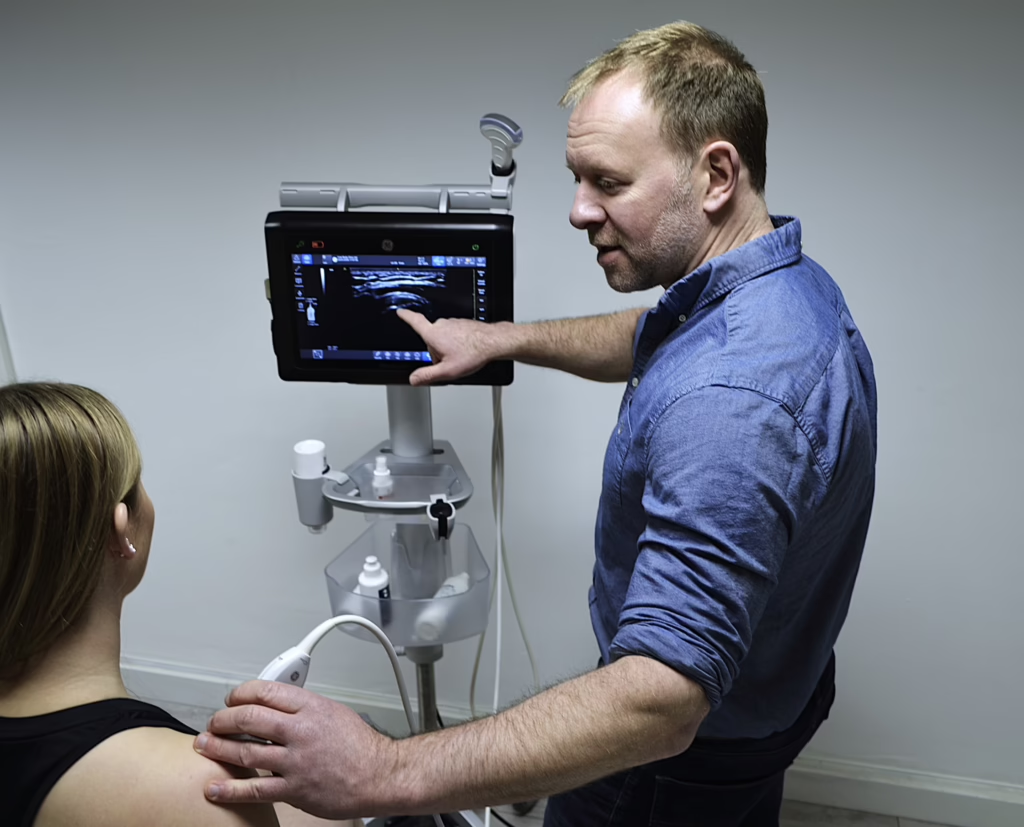
Core Body Clinic is a specialist physiotherapy and sports injury clinic with over 20 years of experience providing expert care and advanced practice physiotherapy in Swansea and Reading. Our philosophy is to provide a one-stop clinic where patients can obtain a complete diagnosis, treatment plan and rehabilitation. Our physiotherapiusts specialise in the treatment of back and body pain, sporting and non-sports related injuries.
yrs
5
Services
Helping You Move Better, Feel Stronger, and Recover Faster
What we treat
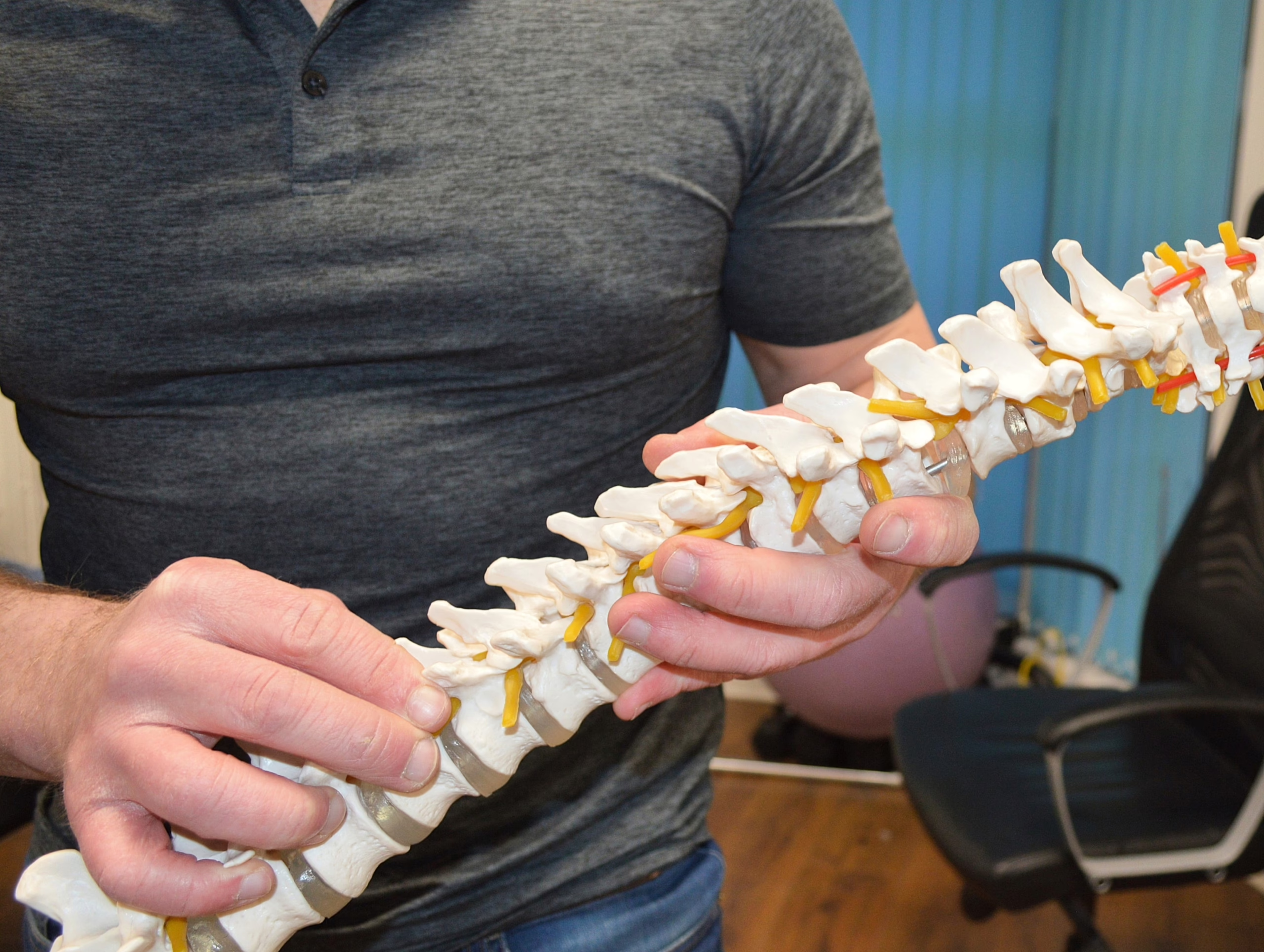
Expert Care For a Wide Range of Conditions
Since 2014, Core Body Clinic Physiotherapy and Health clinic has been providing expert care in Reading and Swansea. Our physiotherapists and clinicians are experts and highly professional in their approach when assessing and treating musculoskeletal problems, sports injuries and pelvic pain.
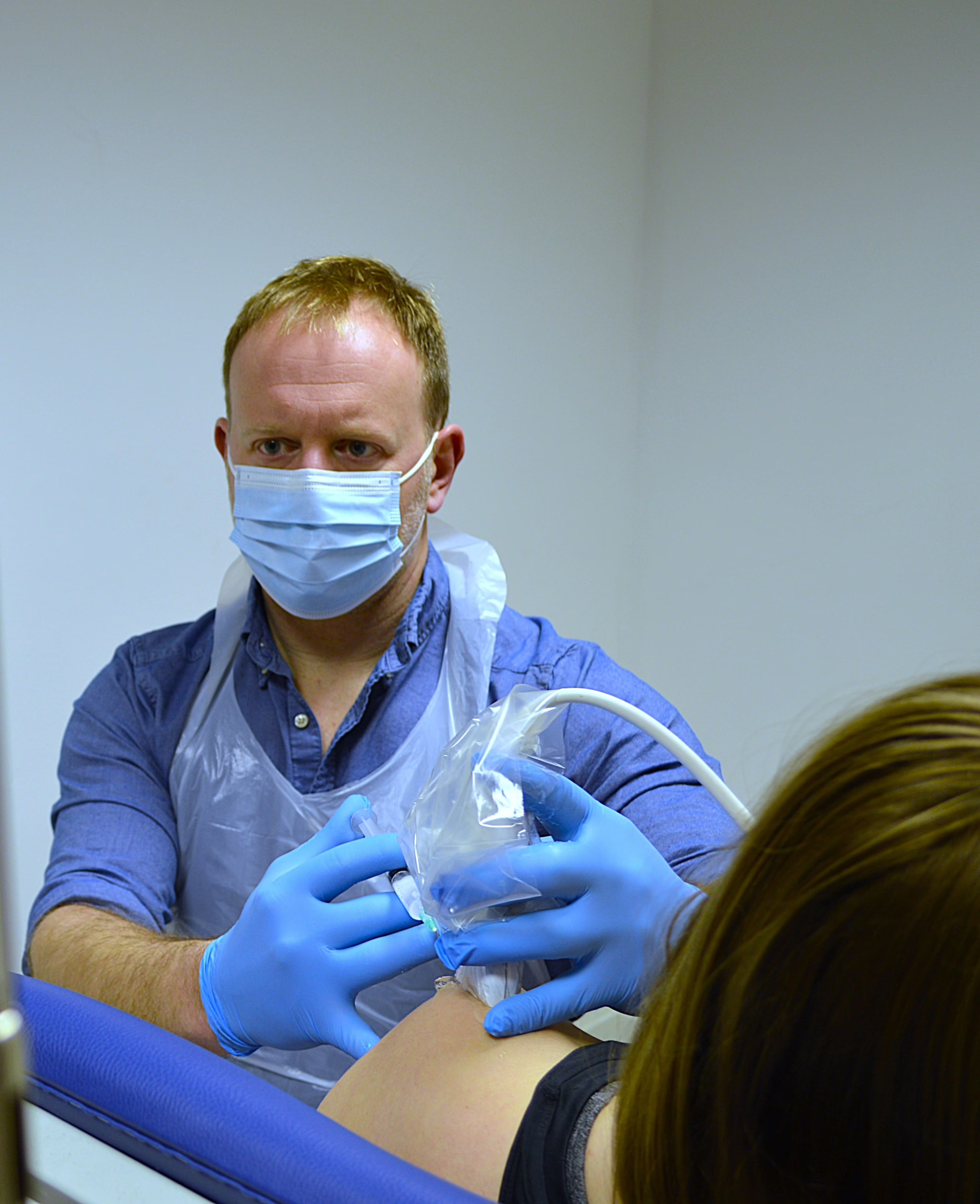
Core Body Clinic is different and uniquely positioned. As advanced practitioners, we offer hands-on physiotherapy, Osteopathy and rehabilitation, combined with ultrasound diagnostics, steroid and hyaluronic injection therapy, shockwave therapy and a men’s health pelvic pain service. This enables Core Body Clinic to function as a one stop health clinic for all your needs.
Meet the team
Meet Our Team of Physiotherapy Experts
Posted onTrustindex verifies that the original source of the review is Google. Arthritic left thumb, this is the second time I’ve been to see Adrian for the same complaint, I would whole heartedly recommend Adrian to anyone, he uses equipment that my local GP doesn’t have, Adrian can accurately locate where the injection is to go. Thank you Adrian 👍Posted onTrustindex verifies that the original source of the review is Google. While having a longish wait for my appointment, I was made welcome and felt listened to. The advice given was clear and the treatment very effective so far. It was less painful than I anticipated.Posted onTrustindex verifies that the original source of the review is Google. The treatment here was outstanding. I had a Hyaluronic Acid injection for my knee arthritis that worked brilliantly. I barely think about my knee now. And whilst I was there, I mentioned I'd had a stiff neck for 4 years and had seen 2 physios, a chiropractor and an osteopath to no avail. Adrian diagnosed and fixed it in one session! I still find it hard to believe. Can't recommend Core Boy Clinic highly enough.Posted onTrustindex verifies that the original source of the review is Google. Very helpful and knowledgeablePosted onTrustindex verifies that the original source of the review is Google. My son(14 years old) was referred to Adrian after weeks of knee pain and injury from football. From the moment we arrived the level of professionalism was outstanding . The knowledge and the way he explained every detail of my sons knee was unbelievable. He's now hopefully on the road to recovery thanks to Adrian . I couldn't reccomend highly enough .Posted onTrustindex verifies that the original source of the review is Google. I can't recommend Adrian enough! I went to the GP etc. and didn't really get anywhere with the pain in my back. After an hour with Adrian he reduced the pain whilst informing me where the pain has come from. With his advice I went from barely being able to get up, to walking with confidence in less than a week. Thanks again.Verified by TrustindexTrustindex verified badge is the Universal Symbol of Trust. Only the greatest companies can get the verified badge who has a review score above 4.5, based on customer reviews over the past 12 months. Read more